GLP-1s, Diabetes, and "Food Noise"
Any successful peptide protocol for weight loss must also include lifestyle changes
If you are diabetic, pre-diabetic, or know someone who has experience with either, then you likely have at least a rough understanding of what causes the disease. It’s an excess of blood glucose — aka sugar in the blood — caused by an inability of the pancreas to produce enough insulin. Insulin is a hormone that helps glucose exit the blood stream and enter cells, where it’s then converted to energy to power the various systems of the body.
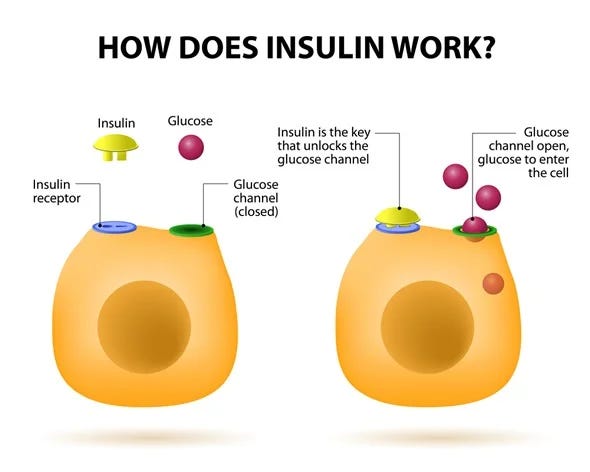
As a diabetic, you’re in a situation where your body is struggling to add kindling to its own furnace. You’re taking in food, which is then broken down into its molecular composites (lipids, sugars, proteins), but is not being efficiently or even correctly appropriated to support your body’s functioning. This is why the unmanaged progression of diabetes mellitus can eventually lead to the deterioration of entire bodily systems (cardiovascular, nervous) and result in major complications like kidney failure, nerve damage, and stroke.
When your doctor prescribes you a GLP-1 like Ozempic (semaglutide), you’re being given a peptide — a complex chain of amino acids — that will function similarly to natural hormones released in the gut directly after we eat. The GLP-1’s effect on the system is fourfold: 1) it triggers the release of insulin from the pancreas so that the recently eaten food can be transformed into cellular energy; 2) it signals for the inhibition of glucagon, which is a blood sugar-raising hormone that counter-regulates the effects of insulin when blood sugar drops too low; 3) it slows stomach emptying, to keep you feeling fuller longer; 4) it sends satiety signals to the Hypothalamic-Pituitary-Adrenal (HPA) axis of your brain, which reduce cravings — aka “food noise.”
The GLP-1 will facilitate bio-regulatory changes in your system that have well known positive effects for diabetics. The peptide will support your pancreas in the manufacture of insulin, which will result in regulated blood sugar, efficient glucose absorption, and vastly reduced risk of cardiovascular or nervous system failure, as well as other complications of diabetes mellitus. Because you are feeling fuller and sated for longer, you will eat less and crave fewer high-sugar and high-fat foods: this will lead to weight loss, which has been demonstrated to improve the prognosis for diabetes patients across the board.
This may sound all well and good — and if you’ve been prescribed a GLP-1 for diabetes, you’re certainly allowed to feel that way — but it’s extremely important that you avoid falling into the trap our diet-forward culture has laid when it comes to just about any weight loss protocol.
Peptide Research, Done Cleanly — Peptide Partners. Independent HPLC/MS, batch COAs, and endotoxin screening to USP <85> validate identity and purity of peptides for research. Browse inventory and view certificates at Peptide Partners.
We at Peptide Partners believe in the responsible, safe, and scientifically sound application of peptide-based health and longevity protocols.
For the diabetic and pre-diabetic — and really for anyone interested in peptide-based treatments for weight loss — this means the following: you cannot treat GLP-1 therapy like a crash diet.
If you want to inject GLP-1s with the goal of suppressing your appetite and losing as much weight as possible as quickly as possible, you certainly can — but that will not be conducive to managing your diabetes. Nor is it what any medical doctor with a competent grasp of the delicate relationships among the endocrine, digestive, cardiovascular, and nervous systems would recommend.
Diabetes is an autoimmune disease, which is a type of disease that results from the body attacking its own healthy tissue, thus impairing its own function. This means that there is no foreign pathogen the body is trying to purge: the disease is simply the result of an overactive immune system. The diabetic body’s autoimmune response happens to be an impairment of pancreatic function.
So, how to mitigate a faulty immune response? The answer does not lie in weight loss alone. Instead of taking the GLP-1 and then starving the body of nutrients — i.e. conveniently forgetting to eat — consider what you could eat that will keep you fuller and more energized for longer.
If you want to see long-term results, you cannot expect to treat GLP-1 therapy like a crash diet.
Think about it: if the semaglutide is increasing the insulin absorption from your bloodstream and sending simultaneous messages to your HPA axis to reduce hunger cues — that would be the “food noise” — then it’s up to you to eat mindfully enough so that you don’t experience a dip in blood sugar, otherwise known as hypoglycemia. Why is this important? If the amount of sugar in your blood gets too low, counter-regulatory hormone glucagon will take effect. That means the inhibition of insulin (something your body already struggles to produce), the powerful signal of hunger cue hormones like ghrelin to summon more food into your system, and the consequent buildup of more blood glucose.
Perhaps you’ve had the experience of trying to regulate your blood sugar and swinging from hyperglycemia to hypoglycemia in the span of a single day. This is not conducive to the long-term treatment of diabetes, and that’s probably easy to recognize when you’re looking at your blood sugar reading or your glucose pump and feeling exhausted by these challenging fluctuations in your body’s chemistry.
But that’s just the thing: successful management of diabetes is all about reducing fluctuations in your blood sugar. This means that no matter what, you need to eat. And maybe now that the GLP-1 has helped reduce your cravings and allowed you to feel sated for longer, those dietary choices will look different. No more skipping breakfast only to correct the resultant blood sugar drop with a high-sugar snack in the early afternoon. Instead, what about eating oatmeal with fruit and yogurt for breakfast, followed by a turkey sandwich on rye and seaweed salad for lunch? What about ensuring that you meet your ideal caloric intake for the day — 1,600 to 2,400 calories for women; 2,000 to 3,000 for men — but by eating food that actually helps the GLP-1 help your body instead of sending your system into a state of starvation for which it will eventually overcorrect?
This is why it’s important to recognize GLP-1s as valuable tools to help you make positive lifestyle changes instead of cure-all silver bullets. Recall that many of the complex amino chains we now know as consumer peptides also occur naturally in the body. The body wants to eat, and it should. All these interventions are designed to help the body’s long-term functioning by mimicking or facilitating chemical reactions, not derailing them.
Sometimes you actually do need to listen to the food noise.


